Asthma Methods
Topic 1: Prevalence
Prevalence is the proportion of individuals in a population who have the disease at a point in time or during a given time period. It is often used to describe the health burden on a given population.
Prevalence is computed by dividing the number of existing cases at a particular point or period in time by the total population from which the cases came. It is often multiplied by 100 and expressed as a percent.
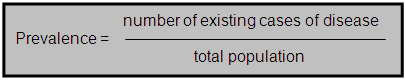
In this report, prevalence estimates are generated in the analysis of data from the Behavioral Risk Factor Surveillance System, School Health Education Profiles, Youth Tobacco Survey, Sentinel Event Notification System of Occupational Risk, and Health Plan and Employer Data and Information Set from the National Committee for Quality Assurance.
Return to top of page
Topic 2: τ-test
The τ-test can be used to compare prevalence measures between two groups. The null hypothesis of this statistical test is that the prevalence for group 1 is equal to the prevalence for group 2; the alternative hypothesis is that the prevalence for group 1 is not equal to the prevalence for group 2.
The resulting p-value of the t-test ranges from 0.0 to 1.0 and gives the probability of finding a significant difference between the two groups when, in reality, no significant difference exists. The standard used to assess the significance of a statistical test is p-value = 0.05. A p value less than or equal to 0.05 indicates that there is at most a 5% chance of observing a difference between the groups by chance alone, given that in reality the prevalence in the groups is similar. In this case, the null hypothesis is rejected and the result is considered statistically significant. If the p value is greater than 0.05, chance cannot be excluded as a likely explanation for the observed difference, so the null hypothesis is not rejected and the result is not considered statistically significant.
The binomial test is very similar to the t-test for comparing prevalence measures between two groups and is interpreted the same way.
Return to top of page
Topic 3: Average
The average estimates a "typical" value for a given continuous variable in a specific population. It is calculated by adding all the observed values of the variable and dividing by the total number of values.
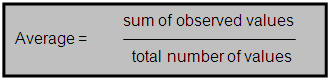
In this report, average estimates are generated in the analysis of data from the Behavioral Risk Factor Surveillance System, Sentinel Event Notification System of Occupational Risk, and Healthcare Cost and Utilization Project.
Return to top of page
Topic 4: Incidence Rate
The incidence rate expresses the rate at which events occur in a population at risk at any given point in time during a defined time period. Rates presented in this report are used to estimate annual incidence for aggregates of individuals, defined by geographic area and demographic characteristics, over a given time period.
The numerator of the incidence rate is the number of new events in the population during a given time period. The denominator is the average population estimated for that same time period multiplied by the number of years in the interval. The use of this denominator assumes that the population and its demographic composition are relatively stable.
The population at the midpoint of a given time interval is used to estimate the average population over the entire interval. This is then multiplied by the number of years in the interval so that an annual rate is generated. For example, to compute a rate of asthma hospitalizations for 1998 through 2000, the population in 1999 (midpoint) multiplied by 3 is used as the denominator. Rates for single years are calculated using the estimated population for that year.

Incidence rates are generally multiplied by a factor of 10 so that they can be better understood in terms of a population. For asthma hospitalizations, rates are multiplied by 10,000, whereas for asthma deaths, rates are multiplied by 1,000,000.
In this report, incidence rates are generated in the analysis of data from the Michigan Inpatient Database, Michigan Resident Death File, and Sentinel Event Notification System of Occupational Risk.
Return to top of page
Topic 5: Age Adjustment by Direct Standardization
Populations often differ in their distribution of age, which may in turn affect the overall rate of events in that population. For example, if one population has a larger number of young children than another, it could demonstrate a higher asthma hospitalization rate simply due to its age structure. Therefore, when comparing rates of events in populations of different age distributions, it is important to account for those differences. In this report, age structure differences are accounted for in overall rates using direct standardization methodology to compute age-adjusted rates. Rates that are not age adjusted are referred to as crude rates.
An age-adjusted rate is a weighted average of age group specific rates in the population under study. The age group specific rates are weighted by the number of people in each age group of a selected standard population. When two or more age-adjusted rates are computed using the same standard population, they may be compared. Age-adjusted rates are presented in this report so that comparisons can be made between geographic subgroups (ex. County vs. County) and demographic subgroups (ex. White vs. Black). The standard population used in the calculation of age-adjusted rates in this report is the 2000 United States Standard Population.
To compute an age-adjusted incidence rate, the first step is to compute the comprising age specific rates. These are then multiplied by the corresponding age specific weight, i.e. the proportion of people in a particular age strata in the standard population. The products of these calculations are then summed and divided by the sum of all the age specific weights.

In this report, age-adjusted rates are generated in the analysis of data from the Michigan Inpatient Database and the Michigan Resident Death File.
Return to top of page
Topic 6: Confidence Interval
The purpose of a confidence interval (CI) is to estimate the statistical uncertainty around a particular measure. For example, the estimated prevalence of asthma among Michigan adults is 8.8%, with a 95% confidence interval of 7.8% to 9.8%; we are 95% confident that the true prevalence in the population is no less than 7.8% and no greater than 9.8%.
In this report, 95% confidence intervals are provided for estimates of prevalence and average annual incidence rates.
The confidence interval formula for an estimate of prevalence is based on the binomial distribution. The upper and lower limits are often multiplied by 100 and expressed as percents.

The confidence interval formula for a crude incidence rate is based on the Poisson distribution. The upper and lower limits are often multiplied by an appropriate factor of 10: 10,000 for asthma hospitalization rates and 1,000,000 for asthma mortality rates.

The confidence interval formula for an age-adjusted incidence rate is based on the Poisson distribution. The upper and lower limits are often multiplied by an appropriate factor of 10 – 10,000 for asthma hospitalization rates and 1,000,000 for asthma mortality rates.

Confidence intervals can be used as a method to test whether a specific measure is statistically different between groups. For example, in comparing a county specific asthma hospitalization rate with that of the State of Michigan, they are considered statistically different if their confidence intervals do not overlap.
Return to top of page
Topic 7: Data Suppression
Incidence rate estimates calculated with a small number of events or population sizes are statistically unstable. They exhibit wide confidence intervals indicative of great variability. In this report, data suppression rules are enforced so that the data presented are reliable. For demographic or geographic subgroups where there is less than or equal to 20 hospitalizations or less than 5000 population, asthma hospitalization rates are not presented. Mortality rates are suppressed when there is less than 5 deaths or less than 5000 population. In addition, to protect the identity of persons who have been hospitalized or died, counts less than 5 are not presented in this report.
Return to top of page
Topic 8: Trend Analysis
To determine if Michigan has experienced an overall trend in asthma hospitalization and mortality rates over the 12-year period 1990-2001, the Spearman Correlation Coefficient and its accompanying statistical Rank Correlation Test were utilized. This test assesses whether there is a statistically significant monotonic relationship between 2 variables, in this case year and rate.
The Spearman Correlation Coefficient (rho, ρ) ranges from –1.0 to 1.0. If the coefficient equals –1.0, it indicates a perfect negative correlation, where each year has a lower hospitalization rate than the previous year. If the coefficient equals 1.0, it indicates a perfect positive correlation, where each year has a higher hospitalization rate than the previous year. As the correlation coefficient approaches 0.0, from either direction, the relationship between the 2 variables weakens. For example, a correlation coefficient of 0.90 indicates a stronger positive relationship between 2 variables than a coefficient of 0.50.
The p-value of the Rank Correlation test ranges from 0.0 to 1.0 and gives the probability of finding a significant overall monotonic trend in the asthma hospitalization rate data when, in reality, no trend exists. Again, the standard used to assess the significance of a statistical test is p-value = 0.05. A p value less than or equal to 0.05 indicates that there is at most a 5% chance of observing a trend, given that, in reality, rates are stable. In this case, the result is considered statistically significant. If the p value is greater than 0.05, chance cannot be excluded as a likely explanation for the observed trend, so the result is not considered statistically significant.
From this, it follows that:
- If there is a statistically significant increase in asthma hospitalization rates over time, the Spearman Correlation Coefficient will be positive and the p-value for the test will be less than 0.05.
- If there is a statistically significant decrease in asthma hospitalization rates over time, the Spearman Correlation Coefficient will be negative and the p-value for the test will be less than 0.05.
IMPORTANT:
This is a crude analysis that simply identifies whether there is an overall increase or decrease in the asthma hospitalization or mortality rates. This statistical test does cannot determine the significance of more complex trend patterns. There is no way to know from these statistics if a specific event or series of events caused an observed change in rates.
Return to top of page
References
Hennekens CH. And Buring JE. Ed. Mayrent SL.
Epidemiology in Medicine. Boston, MA: Little, Brown, and Company, 1987.
Hollander M and Wolfe DA.
Nonparametric Statistical Methods, Second Edition. New York: John Wiley & Sons, Inc., 1999
Klein RJ and Schoenborn CA. Healthy People 2010:
Age Adjustment Using the 2000 Projected U.S. Population. Statistical Notes (20). Department of Health and Human Services. Centers for Disease Control and Prevention, National Center for Health Statistics. January 2001, (http://www.cdc.gov/nchs/data/statnt/statnt20.pdf).
Rothman KJ and Greenland S.
Modern Epidemiology, Second Edition. Philadelphia: Lippincott-Raven Publishers, 1998.
Szklo M and Nieto FJ.
Epidemiology Beyond the Basics. Gaithersburg, MD: Aspen Publishers, Inc., 2000.